New research reveals a critical reason why cancer treatments don’t work for every patient: drugs accumulate unevenly within tumors, often getting trapped inside cellular “recycling centers” called lysosomes. This discovery explains why some cancer cells receive a lethal dose of medication while others are barely affected, even when patients receive the same treatment.
The Problem With Current Cancer Drugs
Recent advancements in cancer treatment, including drugs like PARP inhibitors (used effectively in ovarian cancer), have improved outcomes. However, a significant number of patients either don’t respond to these drugs or develop resistance over time. The key isn’t just whether a drug reaches a tumor, but how it spreads inside the tumor and individual cancer cells.
Researchers at Imperial College London directly observed this process using thin slices of real human ovarian tumors kept alive in the lab. By treating these “explants” with PARP inhibitors, they could track the drugs’ movement through actual tumor tissue.
Mapping Drug Distribution With Advanced Imaging
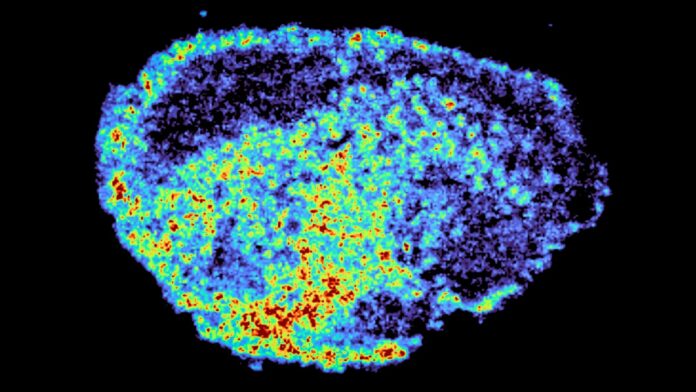
The team used two powerful techniques to visualize drug uptake: mass spectrometry imaging (to map where drugs accumulate) and spatial transcriptomics (to measure gene activity in high- and low-drug areas). The results showed huge variability in drug distribution, even between patients receiving the same dose.
“A novel aspect of this study was the use of mass spectrometry imaging to directly measure and visualize drug uptake in patient tumour tissue. Through the spatial mapping of drug molecules, we could pinpoint regions of high and low drug and compare gene expression, from the same tissue slice, using spatial transcriptomics.” – Dr. Zoe Hall
Lysosomes: Hidden Drug Reservoirs
The research identified lysosomes as key players in this uneven distribution. These cellular structures are designed to break down waste, but some PARP inhibitors get trapped inside, turning them into slow-release reservoirs.
This means that some cancer cells receive prolonged exposure to the drug while others remain largely unaffected. The study found this effect is more pronounced with certain drugs (like rucaparib and niraparib) than others (such as olaparib).
“We were surprised to see large variability in drug accumulation at the single-cell level. This variability was driven by the build-up of a drug in lysosomes, which are acting as reservoirs, increasing the exposure of cancer cells to drugs, by storing and releasing the drug when needed.” – Dr. Carmen Ramirez Moncayo
Implications for Personalized Cancer Treatment
PARP inhibitors are already used to treat ovarian, breast, and prostate cancers, with ongoing trials in other cancer types. Understanding how drugs are stored inside cells could lead to more personalized treatments that maximize effectiveness and minimize resistance.
Researchers hope to identify biomarkers in a patient’s tumor that predict how drugs will distribute, allowing them to tailor therapy accordingly.
Future research will focus on how drug delivery through the bloodstream, tumor structure, and lysosomal storage interact in real patients. This is crucial because tumors in the body have disorganized blood vessels, which could worsen uneven drug distribution.
This study underscores the complexity of cancer treatment and the need for precision medicine. By addressing the underlying reasons why drugs fail, scientists can move closer to more effective therapies for all patients.
The research was funded by the Medical Research Council, Cancer Research UK, the Integrative Toxicology Training Partnership, and the Victoria’s Secret Global Fund for Women’s Cancers.